|
Artistic expression takes on so many different forms: playing an instrument, singing, performing onstage, writing, photography, knitting, sculpting, and the one that likely first comes to mind: painting/drawing. I usually focus on music in this blog, but we can mix it up a little! Therefore, in this post, I would like to share with y’all an artist who was impacted by Alzheimer’s disease: William Utermohlen. Throughout his art career, Utermohlen’s paintings can be categorized into cycles: "Mythological" paintings of 1962-63, the "Cantos" of 1965-1966 (inspired by Dante's Inferno), the "Mummers" cycle of 1969-1970 (which includes characters inspired by the South Philadelphia's New Year’s Day parade), the "War" series of 1972 (referencing the Vietnam war), the "Nudes" of 1973-74, and the "Conversation Pieces" of 1989-1991. Some believed that early signs of Alzheimer’s disease are evident in the “Conversation Pieces,” like shifting spatial perspectives and the focus on an intimate environment. This is evident in Snow, depicted below.  As he aged and after being diagnosed with Alzheimer’s disease in 1995, Utermohlen continued to paint and draw. In particular, Utermohlen focused on creating self-portraits in order to document and express his inner self as Alzheimer’s disease took over his brain. The portraits show grief, pain, resignation, confusion -- it’s heartbreaking to see, but also so valuable in order to get some kind of a sense of the trauma and anguish the person being afflicted is experiencing. Utermohlen’s portraits also show evidence of deteriorating motor functions and spatial awareness, as the lines and facial proportions progressively become less defined. Nevertheless, the portraits help to preserve Utermohlen’s identity, which transcends beyond the physicality of the canvas. This post is only a brief introduction to Utermohlen, and I’d definitely like to share more about him in the future because I find his story and art so inspiring. Next, perhaps I’ll dive deeper into the “Conversation Pieces,” particularly their potential connection to signs of Alzheimer’s disease.
0 Comments
Last but not least, Loma Linda is the fifth Blue Zone. It’s been so interesting exploring these different places around the world, and I hope you’ve enjoyed this series, too! So far, I’ve realized that even though the Blue Zones seem to be quite different in their locations and cultures, they definitely share many characteristics, in both the regions and the ways of life. In my initial impression of all the Blue Zones, Loma Linda stood out as potentially being the most unique, so let’s see if this holds true!
Quick facts: Population: around 25,000 Region type: city Geography: located in San Bernardino Valley, east of Los Angeles Fun fact: the city’s motto is "a city focused on health and prosperity" The aspect of Loma Linda that stands out the most is its large concentration of Seventh-day Adventists. According to Buettner, Seventh-day Adventists “lived between seven and 11 years longer than people in its Northern American counterparts.” In particular, their “Garden of Eden'' diet, which is essentially a plant-based diet, may contribute to a healthier lifestyle. The group also abstains from coffee and alcohol. Perhaps one of the most important practices is sabbath: no matter how busy they are, people will take a break from sundown on Friday to sundown on Saturday to spend time with family, connect with God and nature, self-reflect. This strong connection to church and community is essential in promoting wellness. A strong community has been evident across all the Blue Zones, but a common, specific faith makes Loma Linda particularly stand out. It could be that sharing these beliefs makes community connections run even deeper. Happy New Year, everyone! Thinking back to one year ago, I definitely could not have predicted how this year would turn out. Nevertheless, together, we’ve been able to get through some of the toughest times, and 2021 brings hope for the future. To start off this year’s posts, I will explore the fourth Blue Zone: Nicoya, Costa Rica.
Quick facts: Population: around 161,000 Region type: consists of two provinces (Guanacaste and Puntarenas) Geography: 80-mile long peninsula Fun fact: in Nicoya, men have a higher chance of becoming centenarians than women! Living in a tropical and sunny area could be a factor in the Nicoyans’ secret to living longer. The consistent sunshine helps the body produce vitamin d, which is important in the regulation of calcium and bone health. Furthermore, the water in Nicoya has a very high calcium content, which could also help in creating strong bones and therefore less falls and injuries related to frailty. Diet also contributes to the overall health of Nicoyans. Many Nicoyans follow the Mesoamerican diet, which highlights corn, squash, and beans. Other foods common in this diet include plantains, papaya, pejibaye (peach palm fruit), and yams. All these foods are highly nutritious, providing vitamins and antioxidants. Nicoya shares aspects of lifestyle that are common to most of the Blue Zones so far, like social connections, physical activity, and purpose for living. The concept that Nicoyans embrace is called plan de vida, similar to ikigai in Okinawa. However, such a ‘life plan’ doesn't have to be something grand or exceptional. In fact, most elderly focus on the simplicities of daily life, perhaps teaching their grandchildren about the way of life or checking in on their neighbors, to thrive into old age. Wow, time definitely flies! I can’t believe Thanksgiving just ended, and there’s only about one month until a new year. This year, I’m especially thankful to be healthy. I’m also grateful for this blog, and YOU, reading right now!
Ikaria is the third blue zone I will be discussing in this series, which means this is the halfway point! I think I will continue discussing the Blue Zones in every other post, with a different topic in between. Interestingly so, all the blue zones so far have been islands, including Ikaria. Quick facts:
According to the Blue Zones website, Ikarians are “almost entirely dementia free.” How do they stay so healthy, physically and mentally? A strict mediterranean diet could be a factor. As you are probably familiar, a mediterranean diet consists of many vegetables, fruits, nuts, and whole grains, along with some seafood and poultry. The Ikarian diet focuses more on the plant-based aspects of this diet. Living in a mountainous region, Ikarians get regular physical activity simply by walking up and down the mountainside to a friend’s house or grocery store. Furthermore, Ikarians are very sociable and welcoming, and social connections are definitely important as one ages. Lasting friendships and community bonds have been a common pattern across all the blue zones so far. Another interesting point of study is the shifting through generations. Though Ikaria is isolated, creating a culture and tradition-rich atmosphere, tourism is becoming more popular, influencing people’s way of life. Younger generations could be deviating away from their ancestors’ traditional lifestyle, through adapting modern technology and a mainstream lifestyle. However, genetics also plays a role in longevity, emphasizing the need to take into account many factors with regards to the topic. Nevertheless, I think comparing the lifespans of subsequent generations will be interesting to study and could help provide a picture of the factors that influence longevity to a greater extent. The second blue zone I will be exploring is Okinawa, Japan (the prefecture).
Quick facts:
Okinawa as a blue zone: Okinawa has around 25 centenarians per 100,000, and it’s likely that this number is accurate, as the Japanese government is pretty thorough about the data about its people. Two concepts stood out to be unique to the Japanese and longevity: moai and ikigai. Moai is a group of lifelong friends who support each other in many aspects, from social to financial interests. These groups of friends can last from childhood all the way to the 100s! Throughout their lives, these groups meet, play games, have conversations, just like any other friend group. I think what makes these groups special, though, is the lifelong commitment to each other. Especially throughout childhood, friends usually come and go— we can be close with a couple people in elementary school, but then drift apart in middle school, and that’s the way it is. However, in moais, the friends are committed to one another for life. In a way, these groups are like extended family. Ikigai loosely translates to a reason for being, having a reason to get up in the morning. It seems like gardening is very popular among older Okinawans, which is definitely a reason to get up everyday. Gardening also provides health benefits in itself, providing physical activity and healthy foods. According to Hector Garcia, co-author of the book Ikigai: The Japanese Secret to a Long and Happy Life, “your ikigai is at the intersection of what you are good at and what you love doing.” More specifically, it’s where what you love, what the world needs, what you’re good at, and what you can get paid for converge. At its core, it’s finding meaningfulness in life. These two Japanese concepts place value on living and living into old age. However, what makes Okinawa special compared to the rest of Japan? Ikigai is a popular concept throughout Japan, so perhaps it’s not the main reason Okinawa stands out as a blue zone. However, moai seems to have originated in Okinawa, only gaining attention after Buettner noted it as a characteristic of the blue zone. I also found another interesting characteristic of Okinawa that differs from other places in Japan: uchinaa (Okinawa) time. Contrasting Japan’s precision and punctuality, Okinawans pride themselves on “polite tardiness” and have a forgiving attitude towards being late. I think this may reflect a more relaxed attitude, perhaps related to people feeling less stress. Though, now that I’m thinking about it, if I lived on a tropical island with a group of lifelong friends, I’d definitely be less stressed! As I mentioned in my last post, I will be talking about the five original blue zones for these next couple of posts! The first one is Sardinia, Italy.
Quick facts:
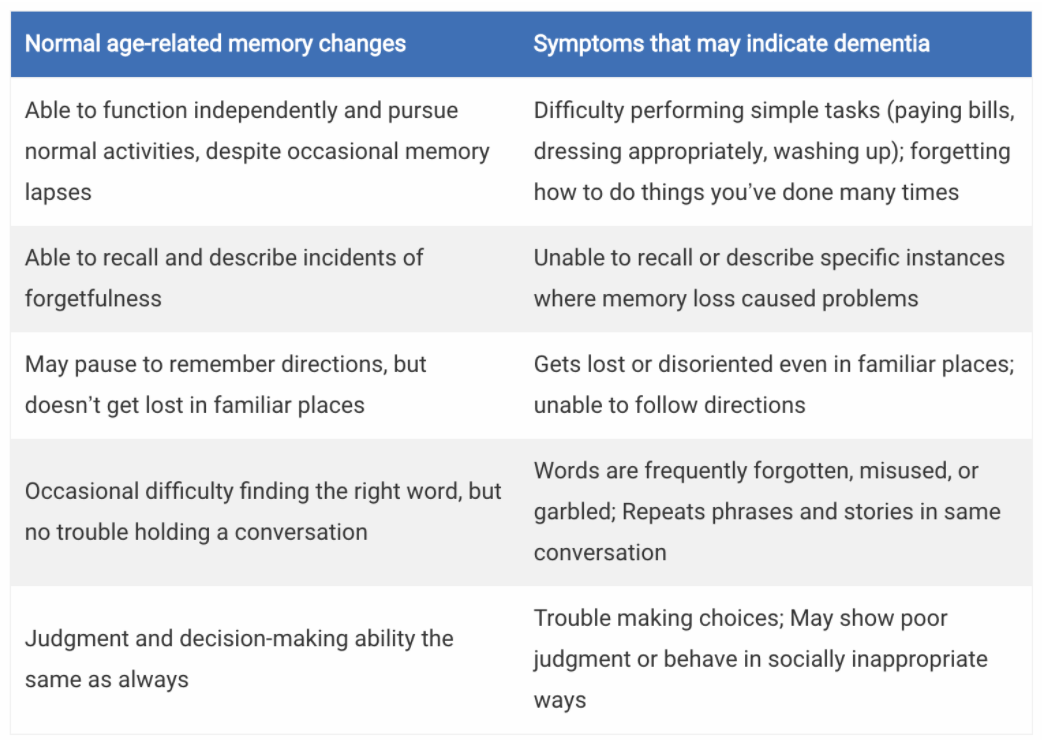
Sardinia as a blue zone: Sardinia was the first blue zone identified by Buettner. His journey to Sardinia was sparked by interest in the M26 genetic marker, which supposedly is related to longevity. I had never heard of this genetic marker myself until researching the blue zones, so I was curious to learn more. However, there doesn’t seem to be much research on it with regards to longevity, making me cautious about the claim. I did find information about a study that found that 150 genes could be related to longevity, and wow, isn’t that a lot! Whether it’s one or many genes, Buettner was led to Sardinia, where he found almost 10x more centenarians per capita than in the United States. A particularly interesting point about Sardinia is that its ratio of male to female centenarians is around 1:1! Some characteristics of the Sardinia lifestyle that’re noted are a plant-based diet with occasional meat, emphasis on family and celebrating elders, walking daily, drinking red wine and goat’s milk, and laughing with friends. I think celebrating the elderly particularly plays a prominent role in their health. The attitude of dismissing the elderly as frail and incompetent, the common view in a society that values youth, has negative impacts to health, both mental and physical. As with anyone being stigmatized, a lowered self-esteem, social isolation, and depression can ensue. Physical health-wise, this attitude can put stress on the elderly, as they’re constantly worried about being a burden to society. The stigma around aging has even been shown to be related to a shorter life. The detrimental effects are nicely summarized in this article, discussing a systematic review done on the health consequences of ageism. Positivity: such a simple concept that can perhaps change the course of our lives. Of course, there are many other variables that contribute to our lifespan, but changing our view of the elderly can be an easy fix, if we set our minds to do so. Supporting the elderly as integral members of society and respecting them for their wisdom can lead to positive impacts on health -- like increased motivation for productivity, stress-free environment -- which may ultimately lead to a longer life. Forgetting: often seen as a sign of aging. But how do we know the difference between “normal” memory loss associated with age and memory loss caused by disease? Why does memory even get worse as we age? Let’s start with the second question. Here are a few potential contributors to our forgetfulness:
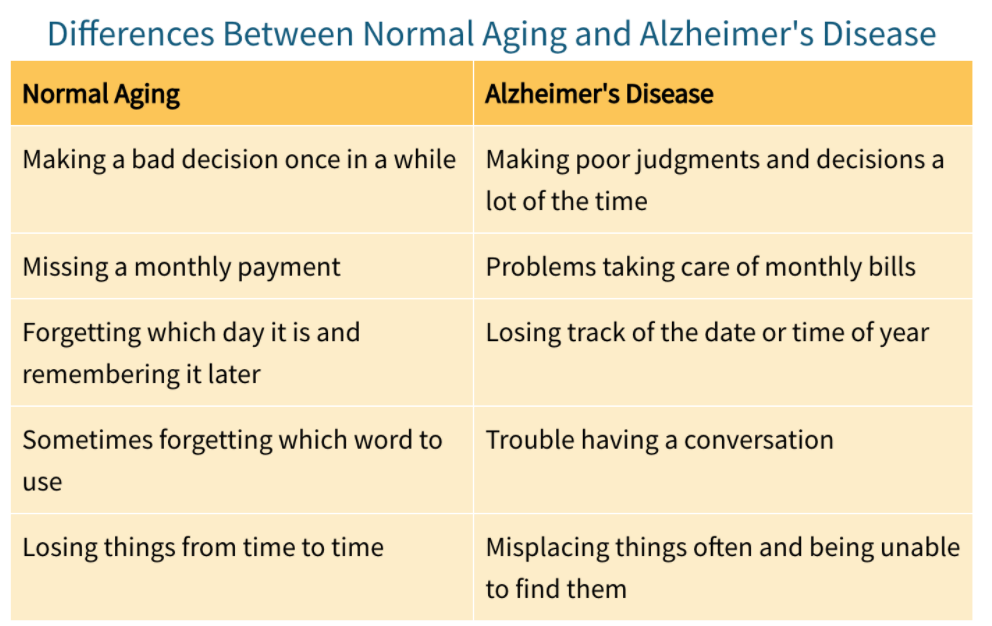
Now for the first question, I found a couple comparison charts that serve as good visualizations, although please keep in mind that everyone's situation is different: Because the brain does change as we age, memory loss could be a part of aging that we can't avoid. However, there are ways to lessen the impact, by ensuring that we are keeping our brains healthy and active for as long as possible. Alzheimer's and other dementias are not a normal part of aging, so it's important to know the differences.
Throughout the United States and across the world, a topic sparking much alarm and urgency is the disproportionate amount of COVID-19 cases in nursing homes and the even larger share of deaths. It breaks my heart to hear the news about these residences being devastated by COVID-19, so I looked into research trying to understand underlying reasons for this. I’ve learned that the inherent characteristics of nursing homes make them more vulnerable: residents likely have underlying medical conditions and the communal setting makes it easier for transmission. Previous research has confirmed that urban location and larger facility size of the nursing home are related to the nursing home having COVID-19 cases. After thinking, this intuitively makes sense: a higher population density makes it harder to social distance, and a larger facility means there’s more traffic of staff in and out of the nursing home. I also watched a webinar hosted by the NIA IMPACT Collaboratory, which affirmed that facilities with COVID-19 cases were likely to be larger, in urban areas, and in states with more cases.
After going through this existing research, I realized most studies are only on nursing homes. What about other types of long term care facilities? Less research has been done on the transmission of COVID-19 in other facilities and comparing the outbreaks to those in nursing homes, although there are many distinctions between the types of facilities, the main one being that nursing homes are more focused on providing medical care for residents. This sparked an idea: I wanted to visualize the different patterns of COVID-19 cases in nursing homes vs other facilities, so I created a map. The map consists of outbreaks in licensed nursing homes and residential care facilities for the elderly (RCFEs; encompass assisted living, memory care, and continuum of care communities) in Los Angeles County, and I also included layers to compare the cases within the racial composition and median income of the area they are located in. The COVID-19 cases are grouped by zip code in order to depict the outbreaks in a community as a whole.
Here is my first map of LA County (the case numbers are not being updated). The nursing home cases are displayed for all of California, while the RCFE cases are only displayed for LA County. To view the legend, click on the arrow button on the top left:
I also recently created a similar map for Austin, TX, with case numbers that are up to date. Here, the exact locations of long term care facilities with cases are displayed: A clear major difference between nursing homes and RCFEs is that there are fewer cases of COVID-19 in RCFEs. I think this could be due to the differences in care and living between nursing homes and RCFEs, like residents being more independent in RCFEs and staff providing less hands-on care. Furthermore, unlike nursing homes, residential care facilities are not federally regulated, but rather states set most regulations, so the quality can greatly vary between facilities. This also means that COVID-19 responses for these facilities can vary greatly between states— yet another factor that could contribute to the presence of COVID-19 cases. Therefore, there may be many more variables to consider with regards to COVID-19 cases in other long term care facilities than in nursing homes. As the extent of the spread of COVID-19 in a community contributes to its transmission into long term care facilities, it is everyone’s responsibility to protect the residents living in them. In order for us to understand this and take necessary precautions, we also need a clear picture of the COVID-19 situation of the long term care facilities in our own communities. Therefore, I believe it’s important to create visualizations of the long term care facility data that are easy and quick to understand and on a local level. This can help the general public to recognize where outbreaks occur, focus appropriate attention and resources, and consciously take action to lessen the spread of COVID-19 to those most vulnerable in the community. Sources
You may be wondering, why am I talking about Australia specifically? Honestly, I chose it because Australia is one of my favorite places I’ve been to, which makes me curious on how the aging care system works there. Who knows, maybe I’ll retire in Australia!
Australia’s aging population: As is the trend in many countries, birth rates in Australia are declining as life expectancy increases. In 2017, 15% of Australians were 65 years old and older. Twenty years later, in 2037, the proportion is estimated to increase to 20%, and in another twenty years, to 22%. With the growing amount of older people, care services for the elderly are becoming important topics of discussion. How does the aged care system work? Here, I will be focusing on the government-funded programs. The main types of care available are residential aged care, home care, and home support. Residential care includes long and short term stays in residential care facilities. The home care program is called Home Care Packages Program (HCP) and provides different levels of care for people in their homes. The home support program is called the Commonwealth Home Support Programme (CHSP) and provides basic care for those who don’t need the full support of home care. In order to qualify for aged care, the individual must be 65+ (50+ for Aboriginal or Torres Strait Islander people) and complete an assessment. Home care: Services provided to help people remain at home include personal care, therapy, food services, home maintenance and modifications, transportation, and more. The CHSP provides services to help people remain independent and safe. HCP is for more intensive care and has different levels, depending on the amount of support needed. Short term care: There are three types of short term care available: restorative, transition, and respite care. Restorative care is for those who are just starting to need help with daily activities. Transition care is for those who are recovering from being in the hospital and integrate back into everyday life. Respite care enables caregivers to take a little break, whether it be a couple hours or a couple days. Long term care: Individuals who can no longer live independently can move into an aged care home, which is basically a nursing home. I like how Australia has two types of care programs for those who want to continue living at home because I think that having a place to call your own home is important in everyone’s lives, but especially for the elderly. This is because in today’s society, aging is often associated with disability. However, even if someone needs help with certain tasks, this doesn’t mean that they are completely incapable or should lose their independence and home completely. In fact, most older Australians do live in their own homes: 73.4% of those 65+ were homeowners in 2011, and only 6.6% lived in residential aged care. It’s important to note that residential care isn’t something totally terrible to avoid, only that it just may not be right for some, like those who enjoy the freedom of living independently. For these people, moving into a facility can be a shock because they’re stripped of their own home, daily routines, and safe place. Along with searching about official aging care services, I also looked at a couple other programs that aim to improve the elderly’s lives. Intergenerational playgroups: This is an interesting model that I came across. In Australia, there are thousands of intergenerational playgroups around the country, with the goal of strengthening ties between generations. These playgroups work by getting 3+ generations together. In long term care facilities, it’s popular for adults to bring their young children to meet with the residents. They all then spend time together, doing activities like singing, painting, and telling stories. I think these playgroups are such a great idea because they benefit everyone involved. For the residents, they are able to socialize and play with the younger generation, which likely helps to brighten their moods and their overall wellbeing. And for the children, they are able to improve social interactions and awareness about the older generation. Be Connected Initiative: This is yet another program helping to connect generations. The goal is to help older adults strengthen their digital skills and online safety. All of its resources are free, including in-person help through the Be Connected Network, which consists of community organizations! In this digital age, it’s important for everyone to be able to access and understand technology. However, the older population is often left behind while the younger generation becomes more fluent and dependent on technology. Another stigma of aging: incompetence with technology. Yes, it may be hard for older people to adapt to technology, as they didn’t have the exposure to such advances growing up, but this doesn’t mean that they can’t learn. I think the Be Connected Initiative can be so helpful for the elderly because through it, they can not only connect to technology, but also with those in their communities through the Be Connected Network. The overall purpose of these two programs that I noticed is connection. As people get older, it does seem like they become disconnected from society, as firstly, they retire and therefore may lose a sense of productivity and purpose, and secondly, society in general is more attracted towards youth. I really think it’s important to address this negative stigma around aging because it’s inevitably going to occur to all of us. By connecting generations through playgroups and technology, everyone involved is able to improve each other’s lives. Sources: https://www.gen-agedcaredata.gov.au/ https://melbourneinstitute.unimelb.edu.au/__data/assets/pdf_file/0010/3398464/HILDA-Statistical-Report2019.pdf https://arc2018.aarpinternational.org/countries/australia https://beconnected.esafety.gov.au/ It’s so crazy to think about how much our world has changed this year. COVID-19 has completely changed the way we interact with each other. Although restrictions are loosening and places are opening up, it’s still necessary to take precautions, especially with the elderly. Today, I want to focus on how COVID-19 affects those with dementia.
There’s no doubt that COVID-19 is especially dangerous for the elderly, but there’s an even higher risk for people with dementia. This is because those with dementia are likely to also have other health problems, like cardiovascular disease and pneumonia, and behaviors related to dementia can increase the risk of them contracting COVID-19. For example, since a characteristic of dementia is memory loss, they may have difficulties remembering safety measures to take, like washing hands or covering coughs. Individuals with more advanced stages of dementia may not fully understand the current situation and risks due to overall cognitive impairment. Those living in long term care facilities are also cut off from their family and friends, which can worsen confusion and stress. Social distancing in general interferes with the social activities, exercise groups, and other types of meaningful activities that are important parts of daily life. Therefore, it’s necessary to provide not only protection against the virus, but also care for mental and physical well being. Both caregivers and patients have roles to play in staying healthy and connected. Here are some examples:
|
Archives
February 2021
Categories
All
|


 RSS Feed
RSS Feed
